`
2
norm error reduction of the residual of = 10
−6
. To illustrate the performance of the
coupling method we consider a system consisting of a 3D EM model of the LV and for the 1D
arterial model we analyse different geometries, either consisting of a single arterial segment
or composed by more complex networks including the major vessels. To reproduce a realistic
case, the LV computational domain is adapted from a patient-specific 3D-whole-heart-MRI
scan collected and post-processed in a previous study, see Figure 1. The biomechanical
3
P H Charlton et al
Figure 1. Simulating PPG pulse waves. (a) The baseline inflow waveform prescribed at the aortic root. (b) The arteries in the 1D
numerical model, showing the sites of PPG pulse wave simulations: the radial, brachial and temporal arteries. (c) Estimating the
PPG from blood pressure (BP). (d) In vivo PPG waves, for comparison.
Figure 2. Simulating pulse waves during mental stress. (a) Prescribed aortic root inflow, Q, waveforms at baseline (black), relaxation
(blue), and stress (red). (b) Prescribed wave speeds, c
d
, of each arterial segment of radius R
d
. (c) Simulated PPG waves at the brachial,
radial and temporal arteries (offset for clarity).
Physiol. Meas. 39 (2018) 054001 (15pp)
3
P H Charlton et al
Figure 1. Simulating PPG pulse waves. (a) The baseline inflow waveform prescribed at the aortic root. (b) The arteries in the 1D
numerical model, showing the sites of PPG pulse wave simulations: the radial, brachial and temporal arteries. (c) Estimating the
PPG from blood pressure (BP). (d) In vivo PPG waves, for comparison.
Figure 2. Simulating pulse waves during mental stress. (a) Prescribed aortic root inflow, Q, waveforms at baseline (black), relaxation
(blue), and stress (red). (b) Prescribed wave speeds, c
d
, of each arterial segment of radius R
d
. (c) Simulated PPG waves at the brachial,
radial and temporal arteries (offset for clarity).
Physiol. Meas. 39 (2018) 054001 (15pp)
3
P H Charlton et al
Figure 1. Simulating PPG pulse waves. (a) The baseline inflow waveform prescribed at the aortic root. (b) The arteries in the 1D
numerical model, showing the sites of PPG pulse wave simulations: the radial, brachial and temporal arteries. (c) Estimating the
PPG from blood pressure (BP). (d) In vivo PPG waves, for comparison.
Figure 2. Simulating pulse waves during mental stress. (a) Prescribed aortic root inflow, Q, waveforms at baseline (black), relaxation
(blue), and stress (red). (b) Prescribed wave speeds, c
d
, of each arterial segment of radius R
d
. (c) Simulated PPG waves at the brachial,
radial and temporal arteries (offset for clarity).
Physiol. Meas. 39 (2018) 054001 (15pp)
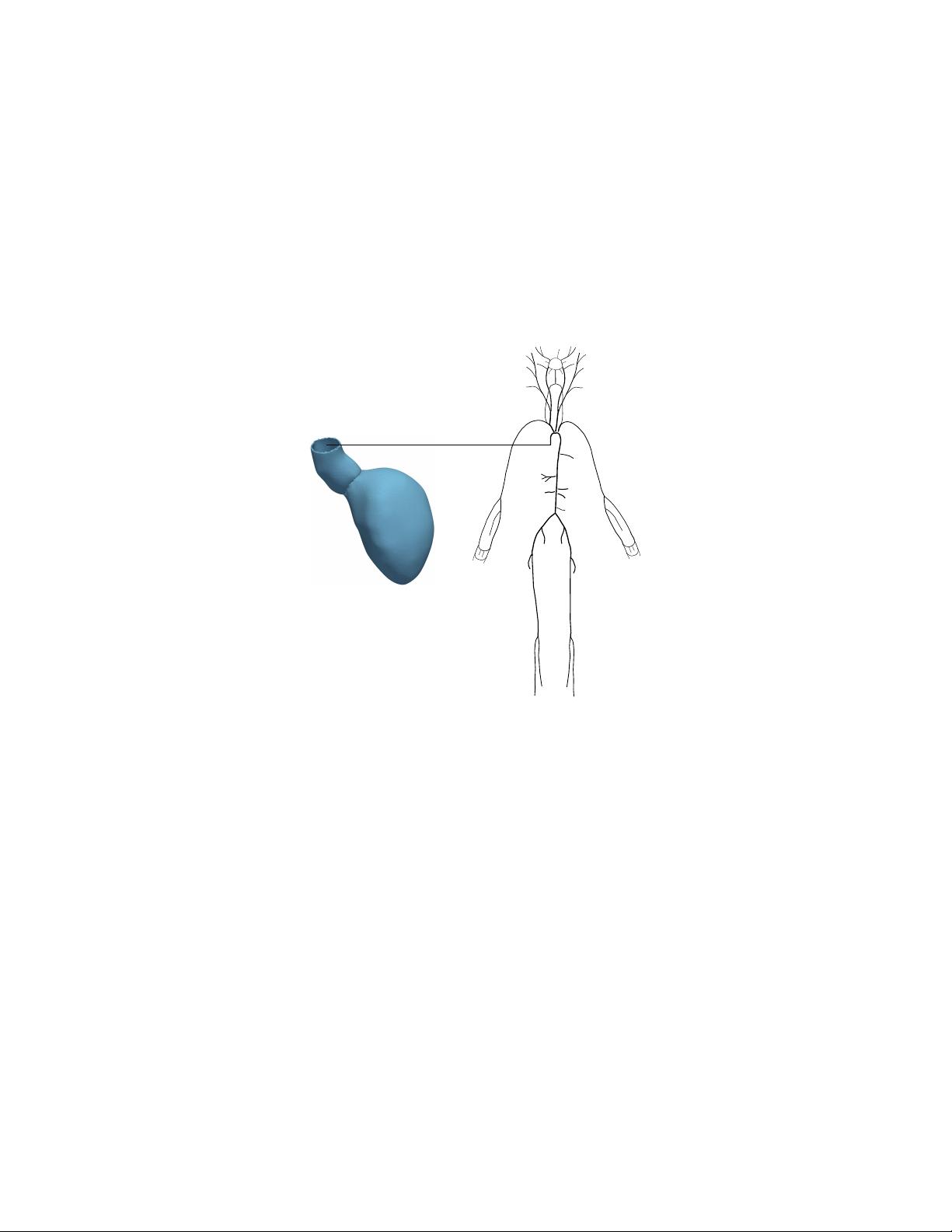
Figure 1: Left: Computational mesh of LV derived from patient-specific image-based clinical data. Right:
1D arterial network.
parameters of the solid and fluid models under baseline conditions have been calibrated to
match a patient-specific set of in vivo measurements at specific instants of the cardiac cycle
for the same subject, see [35] for further information. The same pressure-volume data is
used as for the initialisation of the 3D EM model. All parameters used for the baseline case
are summarised in Table A.1.
9











